DNA Osteoporosis Test
Determine your genetic risk of osteoporosis.
Wondering if you’re giving your bones the care they need? This simple at-home DNA test provides invaluable insights into your genetic risk of osteoporosis and osteoarthritis.- Discover genetic markers associated with bone and cartilage well-being.
- Examine variants in 5 key genes linked to bone health: CYP2R1, GC, WNT16, GDF5, COL1A1
- Gain insights into how specific gene variants can influence your susceptibility to osteoporosis.
- Painless and convenient at-home sample collection.
RM2,330.00
AABB, ISO17025 & CLIA accredited lab
The Science Behind Strong Bones
Our bones are like the framework of a building for our bodies. They support us, anchor our muscles, protect our organs, and store essential minerals.
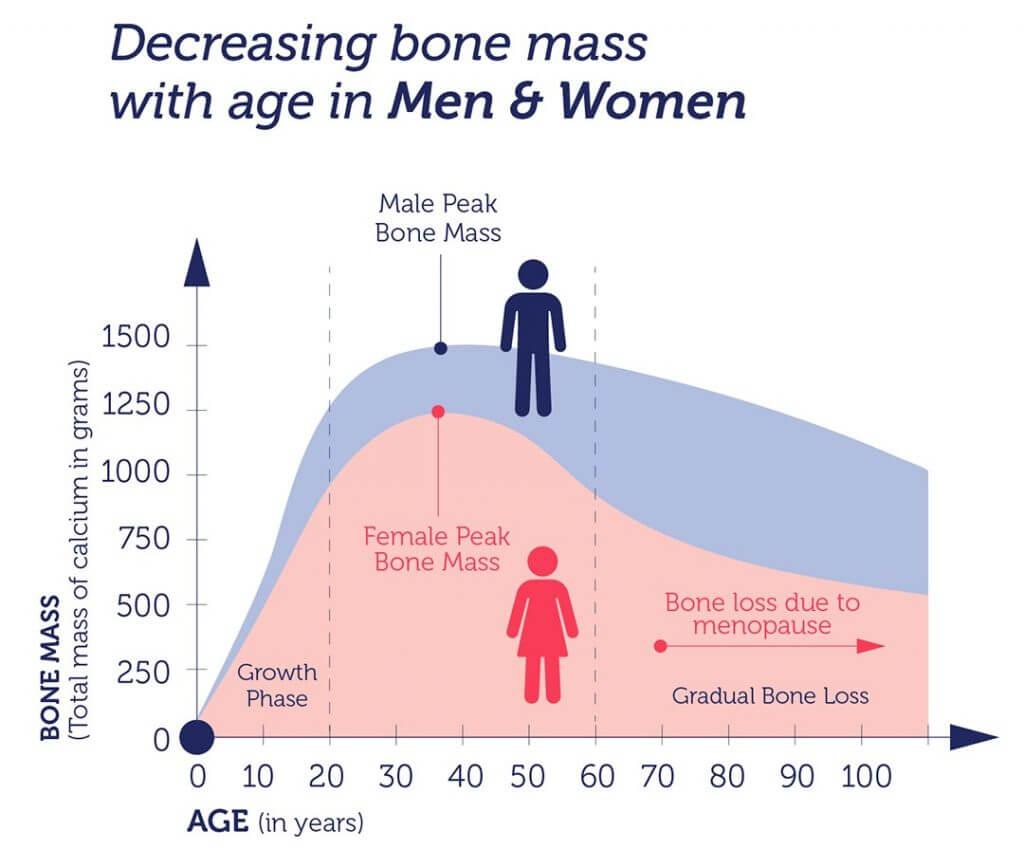
During childhood, teenage years, and early adulthood, our bodies create new bone faster than they break down the old one, reaching the peak of bone strength at around age 30. As we grow older, this balance shifts, with the breakdown of old bone (resorption) outpacing the production of new bone (ossification).
If your bones didn’t grow well when you were younger or you’re losing bone faster than usual as an adult, it can increase your risk of developing osteoporosis.
The Genetics
Your genes offer a blueprint of your bone health. Specifically, the genes CYP2R1, GC, WNT16, GDF5, and COL1A1 give clues about the strength and health of your bones and joints.
Knowing if you’re genetically inclined toward osteoporosis can help you act early. Taking early steps can help fend off bone issues and decrease the chances of severe bone weakening.
Tested Variants
- Vitamin D and Calcium: CYP2R1 and GC are central players. For strong bones, we need calcium. Yet, our bodies depend on Vitamin D to use calcium efficiently. Changes in these genes might affect how our body handles Vitamin D from food and the sun.
- Bone Building Process: The WNT16 gene plays a role in turning specific cells into osteoblasts, the cells that build bones. If this gene isn’t functioning properly, our bones may not be as robust, raising the risk of osteoporosis.
- Bones and Joint Maintenance: The GDF5 gene oversees the health of our bones, joints, and the tissues connecting them. If this gene has issues, it can lead to concerns like joint pain, fractures, or hip problems in children.
- Collagen: The COL1A1 gene contributes to the production of type I collagen, an essential supporting substance in bones and skin. Problems with this gene can weaken bones, a particularly important consideration for women after menopause.
Factors Affecting Bone Health
Strong bones are essential for overall well-being. Here are the primary factors that affect bone health:
- Gender: Women, particularly post-menopause, face a greater risk of osteoporosis.
- Hormones: Men with decreased testosterone levels might experience diminished bone strength.
- Ethnicity: While Hispanics and African-Americans tend to have denser bones, reducing their osteoporosis risk, Caucasians and Asians might be more susceptible.
- Physical Activity: Engaging in weight-bearing exercises like walking, running, or dancing helps reinforce bone strength. On the flip side, a sedentary lifestyle can lead to weaker bones.
- Medications: Prolonged use of certain medicines, such as corticosteroids, can adversely affect bone density.
- Genetics: Specific genes, including CYP2R1, GC, WNT16, GDF5, and COL1A1, have strong links to bone and joint health.
Distinguishing Osteoporosis and Osteoarthritis
While both osteoporosis and osteoarthritis are related to bone health, they have distinct causes and characteristics.
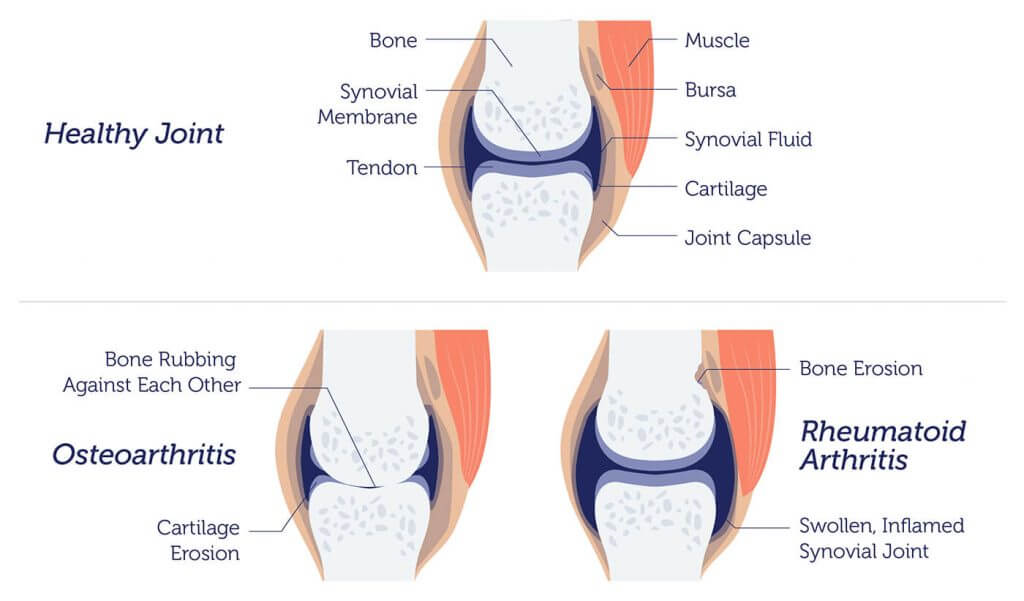
- Osteoporosis: This condition arises when bones lose their strength, becoming fragile and easily broken. Surprisingly, bone fractures resulting from osteoporosis are more common occurrences than heart attacks, strokes, or diagnoses of breast cancer.
- Osteoarthritis: This condition stems from the gradual breakdown of joint cartilage. It’s common in older adults and is the top cause of arthritis.
How Home DNA Testing Works

Order Test Kit
From relationship tests to health tests, we offer a wide range of DNA tests to fit your needs.

Collect & Ship
Collect your DNA with our painless mouth swabs, then send the samples to our laboratory for analysis

Receive Results
Access your confidential results online the moment testing is completed. Our team of experts is available for any questions.
Electronic Reports Delivery